Human Disease
COVID-19 response and recovery
What is a Human Disease Epidemic?
The human population is exponentially growing, and worldwide there appears to be an increase in the reported cases of infectious diseases. Infectious agents vary greatly in size, type as does the method of their transmission. You may have heard of one or two of the many viruses, bacteria, protozoa and multicellular parasites that can cause illness in humans which are almost always transmitted in one of two following forms:
Direct Transmission:
Human to Human – e.g. TB, HIV/AIDS and measles (Also known as Anthroponoses)
Animal to Human – e.g. Rabies (Also known as Zoonoses)
And Indirect Transmission:
Malaria, dengue fever, yellow fever (Also known as vector-borne Anthroponoses)
Bubonic plague and Lyme disease (Also known as vector-borne Zoonoses)
Seasonal viruses (such as influenza) circulate and cause disease in humans every year. In temperate climates, disease tends to occur seasonally in the winter months, spreading from person-to-person through sneezing, coughing, or touching contaminated surfaces. Seasonal influenza viruses can cause mild to severe illness and even death, particularly in some high-risk individuals. People at increased risk for severe disease include pregnant women, the very young and very old, immune-compromised people, and people with chronic underlying medical conditions.
A pandemic occurs when a virus which was not previously circulating among humans and to which most people don't have immunity emerges and transmits from one person to another. These viruses may emerge, circulate and cause large outbreaks outside of the normal influenza season. As the majority of the population has no immunity to these viruses, the proportion of persons in a population getting infected may be quite large.
The World Health Organization (WHO) Director-General is responsible for declaring changes to the global pandemic warnings, following advice from an international expert advisory group.
Why is a Human Disease epidemic an Emergency?
An infectious disease emergency is defined as the occurrence of more cases of an infectious or transmissible disease than would be expected in the State’s population or a sub-group of the State’s population during a given time period, and the management of which requires resources that exceed the capacity of existing health services.
Infectious diseases cause not only suffering and death in both humans and animals, but also have severe economic and social implications, which are not always immediately appreciated.
Outbreaks of an epidemic such as foot-and-mouth disease can lead to the culling of millions of animals, and cost the nation billions in clean up and lost earnings. Outbreaks of this magnitude would also impact areas such as tourism and create economic losses for international exports.
Historically, infectious diseases have had civilisation-altering consequences. For example during the Spanish flu pandemic in 1918–1920, between 50 and 100 million people worldwide were killed by illnesses related to the infection.
Because of the nature of pandemic illness and in spite of the increased attention and the improving knowledge we have on diseases, it is extremely difficult to formulate policies which will reduce the consequences of a large scale outbreak. Improved living conditions and increased access to medications mean the proportion of human deaths caused by infectious diseases has trended downwards over the last centuries, making the occurrence of degenerative and lifestyle diseases more common. However, history has previously witnessed spikes in morbidity and mortality due to infectious diseases and this reduction may not be lasting. The next Pandemic could happen at any time.
Prevention
Roles and responsibilities
The National Strategy for Disaster Resilience, developed by the Council of Australian Governments, provides high-level guidance on disaster management to agencies with a role in emergency management. Foremost in the Strategy is the principle of all of society taking responsibility for preventing disasters.
In the context of Human Disease Emergencies:
Individuals
People should be aware of their own risks and should follow advice from emergency services when responding to warnings. To increase community resilience, individuals should actively plan and prepare for protecting their own life. Resilience is also increased by knowing and being involved in local community disaster or emergency management arrangements, and a volunteer role.
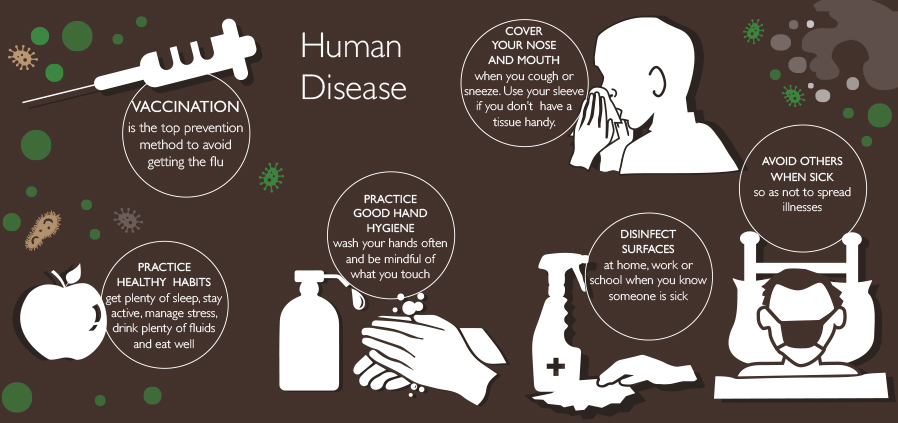
Take these steps to help prevent a health epidemic in your community:
Vaccinate
The immediate benefit of vaccination is individual immunity and a long-term (sometimes a lifelong) protection against a disease. Vaccines recommended in early childhood immunisation schedules protect children from a range of illnesses that can cause disability or death if contracted.
Vaccines can be just as important for adults too, providing immunity to illness in those considered vulnerable to seasonal viruses. Older adults, people with disabilities, and anyone with a pre-existing chronic illness are all recommended to have seasonal vaccinations.
Residents travelling to a foreign country should always review the current health situation in the countries they are visiting a few months before travel to ensure they have time to get vaccinations if needed.
More information on immunisation and Councils immunisation schedule can be found on our Immunisation Webpage or by contacting your local doctor’s surgery.
Practice Healthy Habits
Practice Good Hygiene
Some tips to minimise your risk of infection and also enhance your overall health:
- Bathe regularly with soap. Wash your body and your hair often
- Trim your nails
- Brush and floss your teeth
- Wash your hands
- Sleep well
For most people, good hygiene is so much a part of their daily routine. If you are concerned for those you care about, help them be healthy and safe by practicing good personal hygiene.
For more information on good hygiene habits and food preparation within the local area please visit our Food Hygiene and Safety webpage.
Practice good food safety
Food poisoning occurs through the consumption of disease-causing germs, or their toxins, present in:
- Raw or under-cooked food of any type
- Food contaminated with faecal matter or infected by food handlers
- Untreated contaminated water
Proper food preparation and storage will help prevent food-related illnesses. For more information visit the SA Health Food Safety Webpage
Handling and preparing food
When you handle and prepare food:
- Wash your hands before, and in-between handling raw food and ready-to-eat food
- Wash raw fruit and vegetables well
- Thoroughly cook all food of animal origin, including eggs
- Wash boards and knives in warm soapy water between handling cooked and raw food
- Defrost food by placing it on the lower shelves of the fridge or use a microwave.
Storing Food
If you store food:
- Keep food covered
- Allow cooked food to cool slightly before putting it in the fridge
- Store raw meat, poultry and seafood below cooked or ready-to-eat food
- Keep your fridge clean.
Food temperatures
- Your fridge temperature should be below 5°C
- Keep hot food hot (above 60°C) and cold food cold (at or below 5°C)
- Reheat food until the internal temperature of the food is piping hot
- Before eating microwaved food, make sure it reaches an even temperature
Cover Your Mouth and Nose
Many viruses are passed from one person to the other through fluids from mouth and nose secretions. When we cough and sneeze droplets go into the air, we are essentially ejecting those particles out into the world, free from our bodies, so that they can land on other surfaces or be inhaled by other people.
You should always try to sneeze into a disposable tissue. If you don't have those with you, you should sneeze into the crook of your elbow. This will minimise the chances that you will spread the germs to another person or surface.
Avoid Contact with Sick People
This is quite a simple way of containing a virus. Some viruses can live on a person’s skin and anything they may have touched (such as doorknobs, remote controls and faucet handles) for up to 48 hours.
As it is nearly impossible for a healthy person to avoid touching any of these items it is recommended that you set aside a room for whoever is sick. The sick person can then stay there while getting better. Set up the room with everything they might need, like tissues, medicine, a thermometer and water and limit the amount of physical contact that you have with them as much as possible.
Disinfect Surfaces
If someone in your home is unwell: Wipe hard surfaces, such as counters or tables, clean and then wipe with a disinfecting solution. Dishes (plates, cups, glasses), utensils (knives, forks, spoons), and cooking equipment (bowls, pots, pans) need to be cleaned and sanitized after each use. Use a dishwasher for washing dishes whenever possible. The dishwasher may sanitize with both heat and chemicals.
Insect bites
Insects including mosquitoes, flies, sand-flies, and fleas pass on infectious diseases to humans through the insect's bites. Infectious diseases caused by insects include dengue fever, malaria, Ross River fever and the Zika virus disease. It's important to avoid insect bites at all times. Follow these tips to stay safe:
- Avoid outdoor exposure to insects
- Wear protective long, light coloured, loose-fitting clothing when outdoors.
- Use a personal repellent containing diethyl toluamide (DEET) or picaridin.
- Install insect screens on doors and windows of homes, and on enclosed outdoor recreational areas.
- Use mosquito nets and mosquito-proof tents if camping or living outdoors.
More information on protecting yourself from mosquitoes from SA Health
The World Health Organisation (WHO)
Working through offices in more than 150 countries, W.H.O. staff members work side by side with governments and other partners to ensure the highest attainable level of health for all people.
They work to combat diseases – infectious diseases like influenza and HIV and non-communicable ones like cancer and heart disease. They aim to help mothers and children survive and thrive so they can look forward to a healthy old age and ensure the safety of the air people breathe, the food they eat, the water they drink – and the medicines and vaccines they need.
You can find out more about the W.H.O. by visiting their website
Government agencies, local governments andcommunities
Organisations should include Human Disease Risk within their Community Emergency Risk Assessment activities. This includes consideration within emergency management planning.
Resilience is developed through land management and planning arrangements, assessment of risks, supporting individuals and communities to prepare for extreme events, and having effective education programs available.
Additional prevention tasks carried out by state and local government include:
- Risk assessments to gain an appreciation of human disease risk;
- Engaging with the community regarding human disease risk;
- Working with communities to plan the management of human disease risk;
- Providing emergency information and outbreak warnings;
- Ensuring an effective, well-coordinated response to an human disease epidemic event; and
- Helping communities to recover and learn following an epidemic and build their resilience to future events
The National Framework for Communicable Disease Control is designed to unite government agencies with the goal of strengthening defences against communicable diseases. The framework encourages co-ordinated strategies and is maintained by the Department of Health.
The Office of Health Protection (OHP) is engaged in a range of activities to reduce the incidence, and thereby the social and economic impact of communicable disease. The OHP is the Commonwealth's primary data collection and coordination centre for many communicable diseases. The OHP also coordinates and contracts other agencies to collect data and/or conduct research on communicable diseases.
Vulnerable people
There are many groups of potentially vulnerable people (e.g. older adults, people with disabilities, people living in poverty) whose unique needs may not be accounted for in most emergency plans.
Vulnerable people require more attention when they are experiencing an Emergency situation compared to everyone else. Planning to help friends and relatives who are considered vulnerable contributes greatly to emergency resilience in communities.
Private Industry and businesses
Businesses play a fundamental role in supporting a community’s resilience to disasters. They provide resources, expertise and essential services on which the community may depend. Businesses, including critical infrastructure providers, can also make a contribution by understanding the risks that they face and ensuring that they are able to continue providing services during or soon after a disaster.
Businesses should plan for the risk of disruption, and ensure arrangements are in place to maintain critical services where required.
The links below are designed to help businesses plan for emergency situations:
Business Continuity plans - A quick guide to impact analysis and plan development
Plan and prepare State Government advice on how to protect your business
For additional information about Preventing the spread of human diseases:
Centres for Disease Control and Prevention
The Department of Health
Prepare
Things you can do now to prepare for a Human Disease Epidemic:
Understand your risk
Find out more about potential Biological agents/diseases by following the below links to the NSW Infectious diseases page
Food Safety Threats
Find out more about potential foodborne diseases by following the below links to the NSW food authority page:
Pandemic Preparedness
The South Australian Emergency Management Sector encourages every household, business and farm to have a written emergency plan.
It is worthwhile having a plan for what you would do if your usual ways of getting groceries, petrol or medical supplies are disrupted for several days. Here are some suggestions of things you can do to prepare for a disease outbreak:
- Put together an emergency kit - See our guide in the links section
- Include an emergency pantry supply (aim for 14 days of supplies)
- Learn more about the impacts of a pandemic
- Discuss how your household would manage during a pandemic outbreak
- Identify people you could turn to for help, and others who might need your help
- Investigate your life insurance and income protection policies
Epidemic Notifications
Whilst it is not possible to predict the timing and size of an outbreak, notifications are constantly provided by the World Health Organisation, who analyse and report on disease outbreaks internationally.
The WHO works directly with government agencies for the purposes of providing warnings and alerts to governments, emergency services and the general public in Australia and overseas.
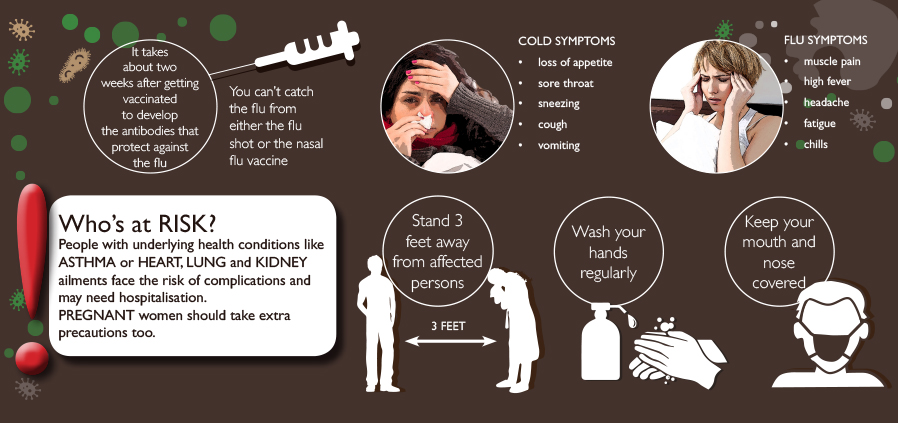
Look out for symptoms and act
In a case of pandemic influenza the main symptoms would be similar to those of seasonal influenza. These usually occur one to three days after infection, and may include sudden onset of:
- Fever
- Headache
- Muscle and joint pain
- Sore throat
- Cough
- Runny or stuffy nose
- Severe tiredness
- vomiting and diarrhoea
It is important to remember that some people can be infected with influenza yet show no or only very mild symptoms. If your health deteriorates considerably or you are having trouble breathing, call: triple zero (000).
If a pandemic phone advice hotline is established, the number will be advertised widely.
Terror Attack
Infectious disease emergencies originating from a criminal terrorist attack or incident will be managed by SAPOL as the controlling agency. Follow all instructions given by emergency services. If you are involved in an incident and you feel unwell, limit the number of people you come into contact with a present yourself to the nearest hospital as soon as possible.
Protect your finances
Emergencies are really expensive and can become a significant long-term burden. To ensure that your finances are safeguarded you can protect your main income source by taking out life insurance and income protection insurance.
Check your insurance cover - A quick guide to understanding Insurance
If you need to travel
Visit your doctor or travel health centre at least eight weeks prior to travelling overseas. They will check if you'll need any vaccinations or medications to reduce your risk from infectious diseases for your travel destinations
The links below will help you further assess your situation and prepare for an Outbreak
Vaccine preventable diseases - Australian Government Website
Immunisation services - SA Health Wesite
Respond
Who do I Contact?
To report an emergency or life threatening situation call 000 (triple zero)
In the event of a severe outbreak SA Health is the primary agency in South Australia responsible for responding to severe infectious disease outbreaks, such as a flu pandemic or food poisoning. However such an event is likely to involve a whole-of-government response.
Further information on who to contact in an Emergency can be found on our printable Emergency Contact List or at the following websites
Control Agency (Response and Recovery) SA Health Hazard Leader (Prevention and Preparation) SA Health
What should you do during a Pandemic Outbreak?
Act Safely: Follow all advice given by response agencies.
If you get sick
If you have flu-like symptoms such as fever, cough and fatigue you can get medical advice from your local Doctor or Health Direct by calling 1800 022 222 who are available 7 days a week, 24 hours.
Stay home if you're sick and even if you aren’t.
Families should also have a plan to take care of children who have to stay home from schools or daycare, as these places will likely be shut down during an outbreak.
Ensure you have sufficient supplies if asked you are asked to stay quarantined at home for a prolonged period of time.
Understand Basic Prevention methods to keep from getting sick
- Avoid close contact with people who are sick.
- When you are sick, keep your distance from others to protect them
- Cover your mouth and nose with a tissue when coughing or sneezing
- Washing your hands often will help protect you from germs
- Avoid touching your eyes, nose or mouth.
- Practice other good health habits. (Sleep, physical activity, plenty of fluids and eat nutritious food)
Plan for service disruption
Plan for the possibility that usual services may be disrupted, including those provided by:
- Hospitals and Doctors
- Banks and Shops
- Utilities providers
- Bus and train services, along with possible fuel shortages
- Boarders may shut to interstate and international travel
- Recreational activities should be postponed
What will The City of Port Adelaide Enfield be doing?
Council has plans in place in the event of a pandemic. These plans include:
- Identifying essential services required in the event that City employee absence (due to pandemic-related illness) affects daily operations.
- Identifying and providing training for employees who will serve in back-up roles, if needed, to ensure The City maintains essential services.
- Working with suppliers to ensure resources are available to support essential services.
Stay informed
- You may be part of a larger evacuation
- Listen to the your local ABC Radio Station check regularly for updates and heed any warnings
- Follow official pages on social media
Industry and businesses
Where possible, employers should enable employees to comply with public health recommendations during a pandemic.
Sick leave and other policies (such as telecommuting, working from home, staggered shifts, and other strategies) should promote and create incentives for workers to stay home if they or a household member becomes sick during a severe pandemic or if well, to report to work.
Well employees should report to work (especially those in health care and other critical infrastructure jobs) to ensure business continuity and the ability to provide care as needed.
Workers should be aware of their employer’s pandemic preparedness plans and other strategies that will promote social distancing at the workplace during a pandemic. Implementing these measures will help to ensure a safer workplace during a pandemic and will mitigate the transmission of disease.
Recovery
All agencies will work in a swift, compassionate and pragmatic way to help communities recover from devastation. Communities will need to learn, innovate and adapt in the aftermath of disastrous events
- Don't move a sick person unless they're in immediate danger
- For life-threatening sickness call 000 (Triple zero).
Vulnerable people
Remember that hospitals, aged care facilities and schools may also be affected by the event and may need the support of the community.
Your own support group of friends, family and neighbours may not be available to you as they could have to manage their own recovery efforts.
First aid skills
In the immediate aftermath of an earthquake event people with first aid skills can become a very important resource for the community.
In the case of a large scale event; State and Local Government resources will be stretched to capacity and support from community members who know first aid will be beneficial for treating many non-life threatening injuries.
Find out more about how you can prepare your First Aid Readiness at the St John website.
Non-government organisations and Volunteers
Many NGO’s organise volunteers during the recovery stages of a disaster and Australians often turn to them for support or advice and the dedicated work of these agencies and organisations is critical to helping communities to cope with, and recover from, a disaster. Australian governments will continue to partner with these agencies and organisations to spread the disaster resilience message and to find practical ways to strengthen disaster resilience in the communities they serve.
If you would like to volunteer to help in any way after a large scale event please contact the City of PAE or the Red Cross
Continue to follow your own emergency plan and until it's safe:
- Help others, including neighbours
- Make use of the supplies from your emergency kit
- Start your recovery
- Seek relocation support from friends and family if your house isn't safe to live in
Protect your finances
There might be financial assistance available from governments and other agencies after an emergency, which is usually small and targeted at immediate needs. Thinking about how you can cover financial losses caused by an emergency will save you a lot of stress and burden.
If you have insurance cover for your income, contact your insurer as early as possible.
National emergency and disaster assistance
The following contact details may be useful:
- Australian Government disaster recovery assistance hotline: 180 2266
- Disaster Recovery Payment – Provides a one-off, non-means tested payment for eligible adults and children who have been adversely affected by a major disaster
- Disaster Assist - Provides information on assistance for current disasters
- National Registration and Inquiry System - NRIS registers, finds and reunites family, friends and loved ones after an emergency. It is managed and operated by Australian Red Cross
- People evacuated in an emergency (or people trying to locate family or friends) can phone the Red Cross Inquiry Centre on 1800 727 077 for callers in Australia or international callers on +61 393 283991
Long Term Recovery
There may be instances where recovery from a disaster can take longer than anticipated.
While no one likes to talk about it, emergencies can cause loss of life. This can have an emotional and practical impact on you and those around you. Ensuring you have life insurance and an up to date Will can help to ease the burden on those left behind.
There may also be things that affect you normal daily routine such as:
School and child care closures
Enforced work place closures
Injury or disability caused by the emergency event
The following Contacts are designed to help those in need through difficult times:
- Kids Helpline Call: 1800 551 800
- Lifeline Call: 131 114
- Mental Health: Assessment and Crisis Intervention Service (ACIS) Opening hours: 24 hours Call:131 465 (state-wide emergency crisis)
Call:+61 8 8394 7011 (for callers outside of South Australia) - Parent Helpline Call: 1300 364 100
- Pregnancy Helpline Call: 1300 139 313
Industry and businesses
If you, your customers or suppliers are affected by the emergency event you should enact your Business Continuity Plan to speed up your recovery.
Certain types of events may cause panic purchasing which could have an adverse effect on area of your business and your ability to re-stock your products through your suppliers. Transport disruptions may also cause delays in supply.
